The Common STD That Can Cause Cancer
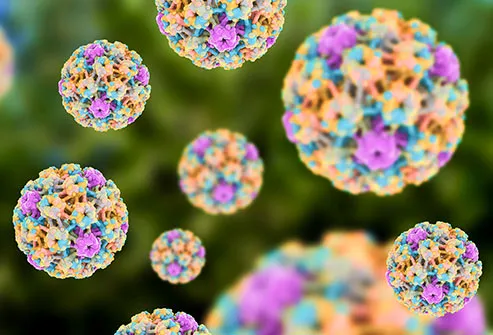
HPV stands for human papillomavirus. It’s a group of more than 150 different kinds of viruses. Some types never cause any problems, while others can lead to health issues, including certain kinds of cancer. You don't always see signs of HPV -- you can have it and not know it.

HPV is spread through skin-to-skin contact. It’s the most common kind of sexually transmitted infection. Almost everyone who’s sexually active will have at least one type of HPV at some point. If your partner has it, you can get it even if they don't have symptoms of it.
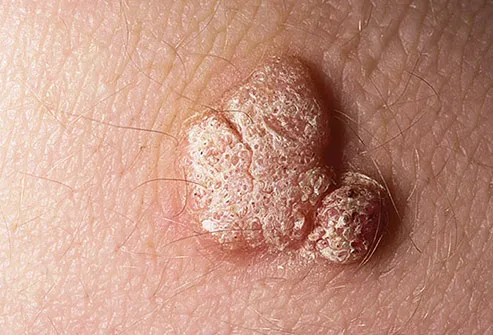
The most common are small, hard sores called warts, but not everyone who has HPV gets them. They may be raised, flat, or shaped like a cauliflower, and they can be different sizes. They can show up on your genital area or other places, depending on the type of the virus you have. These warts often go away on their own. Over-the-counter and prescription drugs can help get rid of them faster, but those can have side effects like swollen or irritated skin.

There’s no cure for these kinds of infections. In most cases, you never even know you had one. If HPV stays around long enough to cause a health problem, your doctor will treat that separately.
About 9 out of 10 HPV infections go away on their own in a year or two. But some of the ones that stick around may cause changes in certain cells that can lead to cancer. This can take 10 to 30 years.
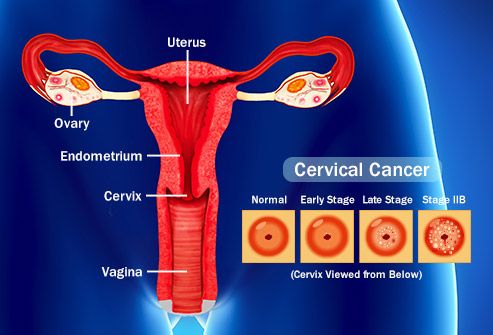
Almost all cases of cervical and anal cancer are caused by HPV. It can lead to it in other genital areas as well, including the vagina, vulva, and penis. About 70% of cases of throat cancer are caused by it, too.

Some things can make you more likely to get cancer because of HPV. These include smoking, taking birth control pills for a long time, and not taking care of your teeth. Your odds are also higher if your immune system is weak or you have chronic inflammation because of another health problem.

The only test for an HPV infection is linked to cancer of the cervix (the tissue that connects the vagina and the uterus). Doctors test for signs of the virus in cells from that area to try to find it before it causes the changes that could lead to cancer. For women 30 and older, this is usually done as part of their annual gynecological exam.
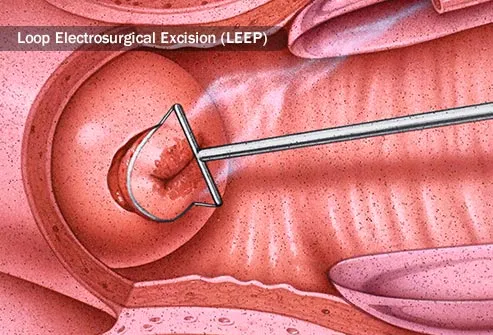
If your doctor finds that HPV has caused changes in some cells that he thinks could lead to cervical cancer, he might use cryosurgery to freeze the tissue that has those problem cells in it. That kills the tissue and keeps the cells from spreading or becoming cancerous. Another option is to take out the tissue. To do that, he might use a small knife called a scalpel, a laser, or a heated wire loop (this is called loop electrosurgical excision).
These are generally treated in the same ways as the ones caused by other things. For example, your doctor might recommend surgery to take out the cancerous tumor. She also might suggest radiation to kill cancer cells and shrink tumors or chemotherapy, a combination of powerful drugs that kill the problem cells.
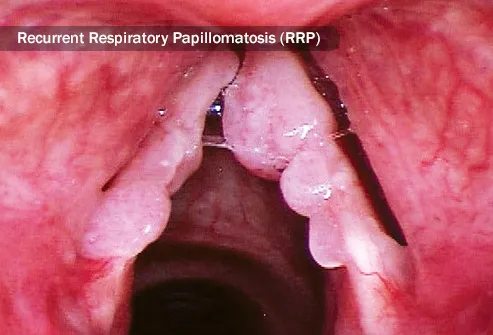
Two types of HPV can lead to a rare disease called recurrent respiratory papillomatosis (RRP). It happens when tumors grow in the airways that connect your nose and mouth to your lungs. They can show up anywhere along this tract, but the ones in your larynx, or voice box, cause the most problems. There’s no cure for RRP. Your doctor can take the tumors out, but they’re likely to come back.
A vaccine can keep you from getting it. It’s best if you’re vaccinated before you’re sexually active so your immune system can be prepared to fight it off. The CDC recommends that girls and boys get vaccinated at age 11 or 12. If you’re older, are already having sex, and have gotten one type of HPV, the vaccine can protect you against other types. So it’s also recommended for men through age 21 and women up to 26. Gay and bisexual men, and anyone with a weak immune system, can be vaccinated through age 26. Pregnant women shouldn’t get the vaccine.

If you’re sexually active, these can help, but they can’t protect you from HPV completely. Areas that aren’t covered by the condom can still be infected. If you’re in the recommended age range, the vaccine is the best way to keep from getting it. But that won’t do anything to fight an HPV you already have.